Delve into the comprehensive world of BeWellSHBP Coverage for Members as we explore the range of services, benefits, and eligibility criteria with a critical eye. Get ready for an informative journey!
Overview of BeWellSHBP Coverage
BeWellSHBP offers comprehensive coverage to its members, ensuring access to a wide range of healthcare services and benefits.
Services and Benefits Included
- Primary care physician visits for preventive care and general health concerns.
- Specialist consultations for specific medical conditions and treatments.
- Prescription drug coverage for medications prescribed by healthcare providers.
- Inpatient and outpatient hospital care for surgeries and medical procedures.
- Mental health services for therapy and counseling sessions.
- Maternity and newborn care for expecting mothers and their babies.
Comparison with Other Health Insurance Plans
When comparing BeWellSHBP coverage with other health insurance plans, BeWellSHBP stands out in terms of its extensive benefits and coverage areas. Unlike some plans that may have limited networks or high out-of-pocket costs, BeWellSHBP provides a wide range of services with affordable co-pays and deductibles.
Additionally, BeWellSHBP prioritizes preventive care and wellness programs to help members maintain their health and well-being.
Eligibility Criteria for Members
To enroll in BeWellSHBP coverage, members must meet specific eligibility requirements set by the program. These criteria are in place to ensure that the coverage is provided to those who truly need it and can benefit from it.
Eligibility Requirements
- Members must be actively employed by an organization that participates in the BeWellSHBP program.
- Members must work a minimum number of hours per week as specified by the program guidelines.
- Dependents of eligible members may also qualify for coverage under certain conditions.
Checking Eligibility Status
Members can check their eligibility status for BeWellSHBP coverage by contacting their HR department or the BeWellSHBP customer service team.
Coverage Options and Plans
When it comes to BeWellSHBP, members have a variety of coverage options and plans to choose from based on their individual needs and preferences.
Different Coverage Options
- Basic Plan: Offers essential coverage with lower premiums but higher deductibles and out-of-pocket costs.
- Comprehensive Plan: Provides extensive coverage with higher premiums but lower deductibles and out-of-pocket costs.
- Family Plan: Allows members to include their family members under one comprehensive plan for added convenience.
Comparing Plans
It is important to compare the different plans offered by BeWellSHBP to find the one that best suits your needs.
- Coverage Limits: Basic Plan may have lower coverage limits compared to Comprehensive Plan.
- Premiums: Basic Plan typically has lower premiums, while Comprehensive Plan may have higher premiums due to more extensive coverage.
- Deductibles: Basic Plan usually comes with higher deductibles, whereas Comprehensive Plan may have lower deductibles.
- Out-of-Pocket Costs: Basic Plan may result in higher out-of-pocket costs for services, whereas Comprehensive Plan may offer more coverage upfront.
Additional Coverage Options
Members also have the option to add additional coverage options or riders to enhance their BeWellSHBP plan.
- Dental Coverage: Members can opt for dental coverage to include routine check-ups, cleanings, and other dental services.
- Vision Coverage: Vision coverage can be added for eye exams, glasses, and contact lenses.
- Prescription Drug Coverage: Including prescription drug coverage ensures access to necessary medications at a lower cost.
Network Providers and Facilities
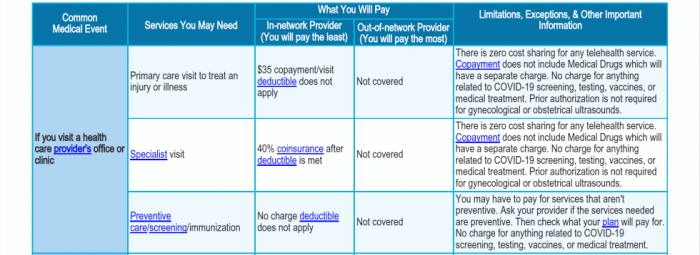
When it comes to accessing healthcare under BeWellSHBP, it is crucial to understand the network providers and facilities covered by the plan. This ensures that members can receive the necessary care without incurring significant out-of-pocket costs.
Network Providers
- Hospitals: Major hospitals in the area are part of the BeWellSHBP network, providing a wide range of medical services.
- Primary Care Physicians (PCPs): Members can choose a PCP from the network to coordinate their healthcare needs.
- Specialists: Various specialists, such as cardiologists, dermatologists, and orthopedists, are available within the network.
Finding In-Network Providers
- Members can easily find in-network providers by visiting the BeWellSHBP website or contacting customer service for assistance.
- Using the online provider directory, members can search for specific healthcare professionals based on location, specialty, or language preferences.
- It is important to confirm the provider's network status before scheduling an appointment to avoid unexpected costs.
Out-of-Network Providers
- Seeking treatment from out-of-network providers may be allowed in certain situations, such as emergencies or when an in-network provider is not available.
- However, utilizing out-of-network services typically results in higher out-of-pocket expenses for members.
- Members should be aware of the associated costs, such as higher deductibles, coinsurance, and potentially balance billing from providers outside the network.
Closing Notes

In conclusion, BeWellSHBP Coverage for Members stands as a robust option with diverse plans and network providers. Make an informed choice for your healthcare needs with BeWellSHBP.
FAQ Corner
What are the eligibility requirements for BeWellSHBP coverage?
Members need to meet specific criteria such as employment status and other conditions Artikeld by the plan. Check with BeWellSHBP for detailed eligibility requirements.
What additional coverage options can members add to their BeWellSHBP plan?
Members may have the option to add riders for dental, vision, or other specific healthcare needs beyond the standard coverage. Consult BeWellSHBP for available add-ons.
How can members find and access in-network providers under BeWellSHBP?
Members can typically search for network providers through the BeWellSHBP website or contact customer service for assistance in finding healthcare facilities within the network.
What is the process for seeking treatment from out-of-network providers under BeWellSHBP?
Seeking treatment from out-of-network providers may result in higher out-of-pocket costs for members. It's important to review your plan's coverage details before seeking care outside the network.