As Options Wellbeing and Integrated Care Models takes center stage, this opening passage beckons readers with a glimpse into a world of innovative healthcare solutions. Dive into a realm where integrated care models and patient wellbeing intertwine to create a holistic approach towards healthcare delivery
This paragraph sets the stage by introducing the key components of effective wellbeing programs, the role of technology in enhancing integrated care, and the importance of addressing social determinants of health in the context of integrated care models.
Options for Wellbeing and Integrated Care Models
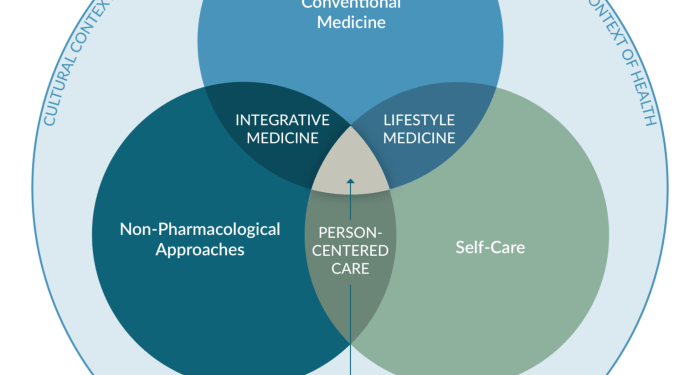
Integrated care models in healthcare involve the coordination of services across different healthcare providers to ensure seamless and continuous care for patients. By breaking down silos between different healthcare professionals and organizations, integrated care models aim to improve the overall patient experience and outcomes.
Examples of Successful Integrated Care Models
- Accountable Care Organizations (ACOs) - A network of healthcare providers that work together to coordinate care for a specific population of patients, focusing on improving quality and reducing costs.
- Patient-Centered Medical Homes (PCMHs) - Primary care practices that provide comprehensive and coordinated care to patients, emphasizing a team-based approach and patient engagement.
- Integrated Behavioral Health Models - Incorporating mental health and substance abuse services into primary care settings to address the holistic needs of patients.
Benefits of Implementing Integrated Care Models for Patient Wellbeing
- Improved care coordination and communication among healthcare providers, leading to better outcomes for patients.
- Enhanced patient experience by reducing fragmentation in care delivery and ensuring a more holistic approach to treatment.
- Increased efficiency in healthcare delivery, potentially lowering healthcare costs and reducing unnecessary services.
Challenges Faced When Implementing Integrated Care Models
- Lack of interoperability between different electronic health record systems, hindering seamless information sharing among providers.
- Resistance to change from healthcare professionals accustomed to traditional care delivery models.
- Difficulty in aligning financial incentives and reimbursement structures to support integrated care efforts.
Components of Effective Wellbeing Programs
Effective wellbeing programs typically consist of several key components that work together to promote overall health and wellness. These components may vary depending on the specific needs of the individuals or groups participating in the program. Here are some essential elements commonly found in successful wellbeing programs:
Wellness Assessments and Goal Setting
Wellbeing programs often begin with comprehensive wellness assessments to identify areas of improvement and set achievable goals. These assessments may include physical health screenings, mental health evaluations, and lifestyle surveys to provide a holistic view of an individual's wellbeing.
Educational Workshops and Resources
Providing participants with access to educational workshops, seminars, and resources can empower them to make informed decisions about their health. Topics may include nutrition, stress management, exercise, and mindfulness practices to promote overall wellbeing.
Physical Activity and Fitness Programs
Regular physical activity is crucial for maintaining both physical and mental health. Wellbeing programs often incorporate fitness classes, group workouts, or access to gym facilities to encourage participants to stay active and improve their overall fitness levels.
Mental Health Support Services
Integrating mental health support services into wellbeing programs is essential for addressing the emotional and psychological needs of participants. This may include access to counseling, therapy sessions, support groups, and mental health resources to promote emotional wellbeing.
Healthy Eating and Nutrition Guidance
Nutrition plays a significant role in overall health and wellbeing. Wellbeing programs may offer nutrition counseling, meal planning assistance, cooking classes, and access to healthy food options to help participants make better dietary choices and improve their overall health.
Social Support and Community Engagement
Building a sense of community and social support is important for overall wellbeing. Wellbeing programs that encourage social interactions, group activities, and community engagement can help participants feel connected, supported, and motivated to maintain healthy habits.
Regular Monitoring and Feedback
Effective wellbeing programs include mechanisms for monitoring participant progress and providing feedback on their goals. Regular check-ins, progress assessments, and feedback sessions help individuals stay accountable, track their progress, and make necessary adjustments to achieve their wellbeing goals.
Role of Technology in Enhancing Integrated Care
Technology plays a crucial role in enhancing integrated care models by improving coordination among healthcare providers, optimizing care delivery, and enhancing patient outcomes. In this section, we will explore the impact of technology on integrated care services, including telemedicine, data analytics, and health information systems.
Improving Coordination Among Healthcare Providers
Technology enables healthcare providers to communicate and collaborate seamlessly, leading to better coordination in integrated care models. Electronic health records (EHRs) and secure messaging platforms allow real-time sharing of patient information, ensuring that all providers involved in a patient's care are on the same page.
Impact of Telemedicine on Integrated Care Services
Telemedicine has revolutionized integrated care by enabling remote consultations, monitoring, and follow-ups. It allows patients to access care from anywhere, reducing barriers to receiving timely treatment and improving overall health outcomes. Telemedicine also facilitates virtual multidisciplinary team meetings, enhancing collaboration among providers.
Data Analytics in Optimizing Integrated Care Delivery
Data analytics tools help healthcare organizations analyze large datasets to identify trends, patterns, and areas for improvement in integrated care delivery. By leveraging data insights, providers can personalize treatment plans, predict health outcomes, and optimize resource allocation for better patient care.
Health Information Systems Supporting Integrated Care Initiatives
Health information systems like interoperable EHRs, population health management platforms, and care coordination software play a vital role in supporting integrated care initiatives. These systems streamline information exchange, enable care continuity across different settings, and empower providers to deliver coordinated, patient-centered care.
Addressing Social Determinants of Health in Integrated Care
Addressing social determinants of health is crucial in integrated care models as these factors significantly impact an individual's overall well-being and health outcomes. By recognizing and addressing social determinants, healthcare providers can offer more holistic and effective care to their patients.
Importance of Addressing Social Determinants of Health
It is essential to incorporate social determinants of health into care plans to ensure that patients receive comprehensive support beyond just medical treatment. Factors such as access to healthy food, safe housing, education, and social support networks can greatly influence health outcomes.
Strategies for Incorporating Social Determinants of Health into Care Plans
- Conducting screenings to assess patients' social needs and connecting them with relevant resources.
- Collaborating with community organizations to provide social support services.
- Developing care plans that address both medical and social needs of patients.
- Training healthcare providers on the importance of social determinants of health and how to integrate them into care.
Role of Community Partnerships in Addressing Social Determinants of Health
Community partnerships play a vital role in addressing social determinants of health as they allow healthcare providers to connect patients with resources and support within their community. By working together with local organizations, healthcare providers can create a more comprehensive approach to care.
Examples of Successful Interventions Targeting Social Determinants of Health
- Providing transportation services for patients who lack access to reliable transportation for medical appointments.
- Offering nutrition education programs and access to healthy food options in underserved areas.
- Partnering with housing agencies to ensure patients have safe and stable housing conditions.
- Establishing support groups and mental health services to address social isolation and emotional well-being.
Closing Summary
In conclusion, the discussion on Options Wellbeing and Integrated Care Models showcases the intricate balance between technology, patient care, and community involvement. By embracing a comprehensive approach, healthcare providers can pave the way for a brighter and healthier future for all individuals.
FAQs
What are some challenges faced when implementing integrated care models?
Challenges may include resistance to change, interoperability issues between different healthcare systems, and the need for strong collaboration among various healthcare providers.
How can social determinants of health be incorporated into care plans within integrated care settings?
Healthcare providers can assess patients' social needs, collaborate with community resources, and tailor care plans to address social factors affecting health outcomes.
What role does data analytics play in optimizing integrated care delivery?
Data analytics helps healthcare providers identify trends, track patient outcomes, and make informed decisions to enhance the effectiveness of integrated care services.